“At the individual level moral distress may cause burnout, lack of empathy, and job dissatisfaction, while at the organizational level it may lead to reduced quality of care, increased staff turnover, and poor patient outcomes.”
Moral distress is essentially knowing the right action to take, but being unable to take that action due to external conflicts. For instance, in therapy we may believe that a patient only requires one visit per week, but the corporation may place pressure on the therapist to see the patient more often during the week. Again, this decision may be due to corporate pressures to make more $$$. If you are the therapist, you are now in the middle of doing the right thing by the patient (at least what the therapist believes to be the right thing) and doing the right thing by the company.
You can see a quick link here speaking to some of the pressures felt by staff PT’s to keep patients longer than “needed”, in the therapist opinion.
When employees feel this pressure, they start to believe that the initial reason for getting into healthcare, “to help people”, becomes trumped by the need to make more money for the company. This difference of personal moral code and corporate code has been shown to lead to moral conflict.
Can you see how this could lead to staff turnover? Of course, when the therapist’s personal mission is not in alignment with corporate mission, it may cause the therapist to find a new job that best matches personal mission. It has been said that Millenials are very concerned about a corporate mission matching a personal mission.
One can logically make the jump from a lack of empathy (not listening or understanding the patient’s position) and job dissatisfaction to worsening clinical outcomes. All of this makes sense to me.
“Generally, resilience refers to ‘the ability to recover or healthfully adapt to challenges, stress, adversity, or trauma'”
I love using this when talking to patients about tissue ability to absorb force and unexpected events. When talking about moral issues, it has to do with a person or therapist’s ability to absorb stress without significant setbacks in emotional or physical well-being.
The article went on to create recommendations for addressing moral distress and moral resilience.
“Institution leaders need to value and create a culture of ethical practice and commit resources to support individuals in cultivating moral resilience”
Many statements can sound great, but creating a culture of ethical practice may be near impossible in all practices. From the top there is a culture that leaks downwards onto the worker bees. This company will assume the “culture” of the owner, if not in whole, at least an iteration of the owner. This is where I believe that having a thorough understanding of one’s own personal mission is vital because otherwise one may assume another’s mission and waste years or decades on a mission that one doesn’t own.
“Encourage accreditation bodies to mandate that curricula for all health care professions include content addressing ethics, moral distress, and moral resilience”
I fully disagree! Whaaat?!
I don’t think that the curricula should include ethical content, but ethics has to be embedded within all of the curricula. Here’s my rendition of an ideal program set-up. The ideas on the periphery can always change, but they must center around creating an ethical professional.
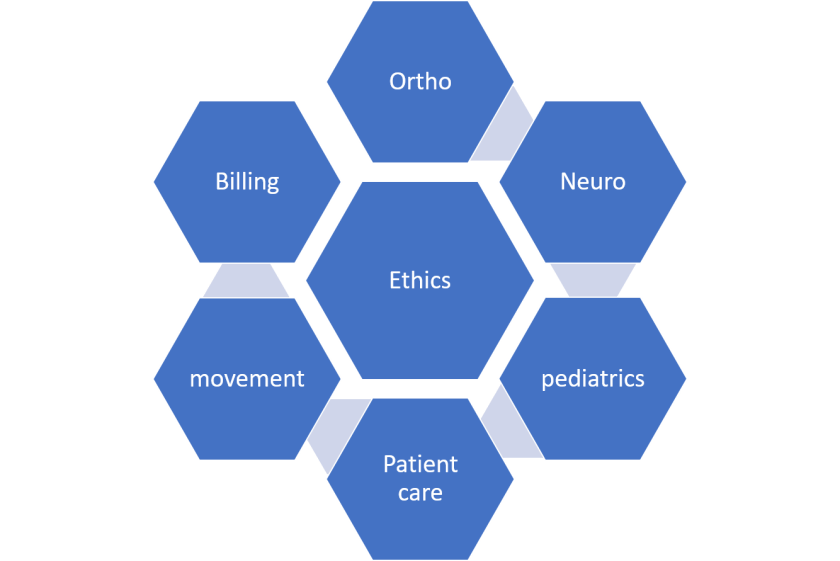
The ethical issues that are noted across the lifespan will differ and the ethical issues noted in business are a completely different animal. Because of this, it is important that topics are brought to the students attention so that they have some background from which to make a decision.
I also don’t think that this should be taught by the professors at the universities. In terms of treating in the trenches, most of academia that I come in contact with haven’t practiced full time in a clinic in a long time or ever. Because of that, there is a lack of “street cred”. It’s hard to discuss and own a topic if there is no experience in the topic.
We had a teacher in PT school that would always say refer to Reese and Bandy (authors of a book), whenever we brought a question. At first, I thought that she wanted us to obtain the answers for ourselves, but over time I learned that the professors (plural) teaching that class 1. didn’t know what was in the book and 2. couldn’t rationalize the ideas that were in the book. They had me refer to a different teacher altogether in order to have him explain the concepts in the book that were contradictory.
Ethics has to be taught from experience…in my opinion.
Excerpts from:
Rushton CH, Schoonover-Shoffner K, Kennedy SM. Executive Summary: Transforming Moral Distress into Moral Resilience in Nursing. AJN. 2017;117(2):52-56.